Alana Korol
 Delving Into The Development Of A Common Skin Condition
Delving Into The Development Of A Common Skin Condition
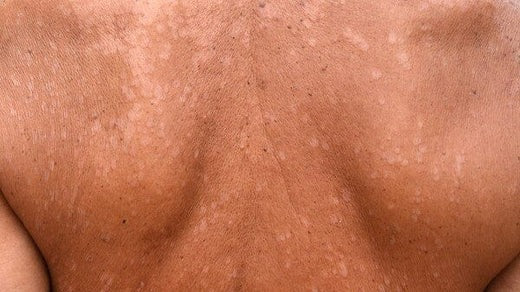
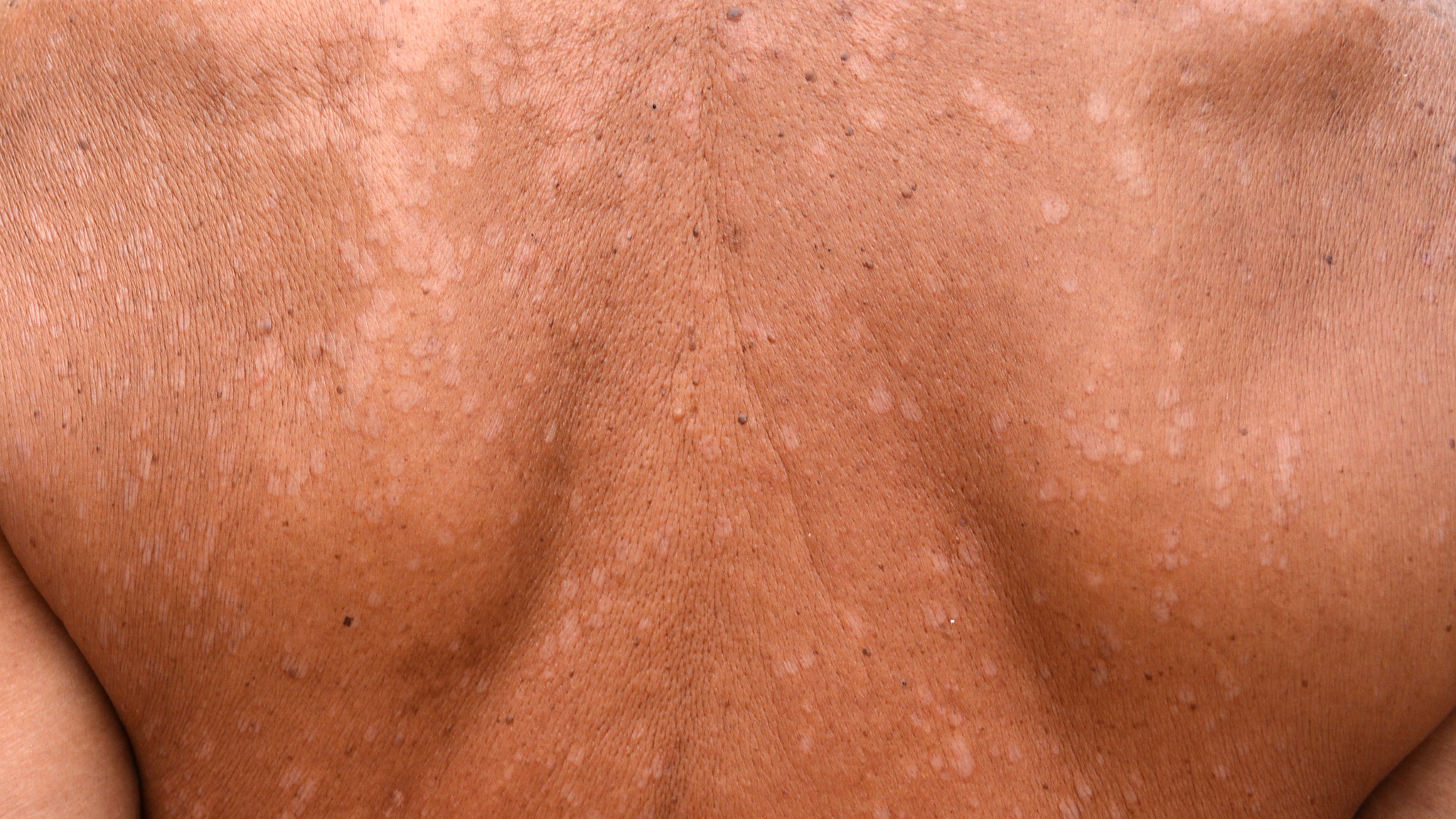
Tinea Versicolor – A Brief Exploration
The Environmental Connection To Tinea Versicolor Outbreaks
One of the biggest misconceptions regarding Tinea Versicolor is the belief that this condition only afflicts those with health complications. While those with specific health issues may be more vulnerable to an outbreak, which is discussed below, most Tinea Versicolor infections directly result from environmental influences. According to leading health organizations, such as the American Academy of Dermatology and the American Osteopathic College of Dermatology, the onset of this fungal infection is due to hot, humid climates. Those living in tropical areas are significantly more likely to suffer from fungal overgrowth than those in dry locations. The primary reason for this result is the biological preference for yeast and skin flora. Without access to dry air, the fungus can reproduce rapidly.
Without a natural balance between dry and wet air, this skin fungus establishes colonies throughout the surface of your skin. Unchallenged, these colonies proliferate at such a rate that the human body cannot contain its progression. Over time, and without effective treatment, the accumulation of this yeast results in skin discoloration caused by the release of azelaic acid, which hinders natural melanin production by inhibiting the release of a specialized enzyme known as tyrosinase. Therefore, those in humid, tropical climates must actively protect their skin by applying anti-fungal creams or natural anti-fungal soaps. This is especially vital for persons who've already experienced a Tinea Versicolor outbreak.
Genetic Predisposition – Biological Factors For Tinea Versicolor
As mentioned earlier, just because you are relatively healthy does not mean you are immune to a Tinea Versicolor infection. The majority of cases are among healthy people. This being noted, several conditions may predispose you to a Tinea Versicolor outbreak. These include:
Excess Skin Oil Production: Those with naturally oily skin are statistically more likely to suffer from an outbreak. When the skin is continuously moist with oil, fungus colonies can thrive and overgrow. Because of this, Tinea Versicolor is a common affliction for teens and young adults.
Excessive Sweating: Men and women who suffer from excessive sweating, such as hyperhidrosis, or hormonal-based sweat production, such as from menopause, are much more likely to develop this condition.
Hormonal Changes: Yeast and skin flora thrive based on various hormonal factors. When a shift occurs in hormone production and concentrations, the delicate balance keeping yeast levels in check becomes altered. In many cases, this results in the overproduction of skin flora.
Suppressed Immune System: Those suffering from a suppressed immune system caused by a medical condition or medication are statistically more likely to suffer from a Tinea Versicolor infection. According to The Merck Manuals, diseases such as diabetes, malnutrition, pregnancy, and HIV/AIDS directly suppress the immune system, which increases the likelihood of developing Tinea Versicolor.